Endometrial Cancer Treatment
I often meet women who are surprised to learn that they have endometrial cancer. While it is not among the most common cancers in women, it is also not extremely rare—and when detected early, it is usually highly treatable. My role is not just to treat the disease, but also to guide you with clear, compassionate explanations, so you feel confident and supported at every step.
In this article, I will walk you through what endometrial cancer is, how we diagnose it, the treatment options available, and the kind of support you can expect—so that you or your loved ones can face this journey with strength and clarity.
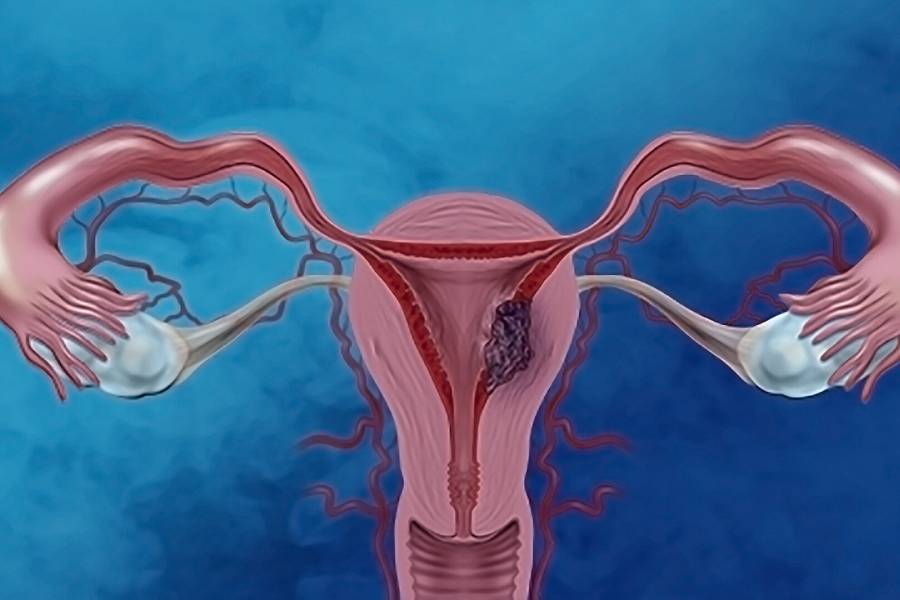
What Is Endometrial Cancer?
Endometrial cancer starts in the lining of the uterus, called the endometrium. It is the most common type of uterine cancer and usually affects women after menopause.
The good news? When caught early, endometrial cancer is highly treatable.
As a Gynaecological Cancers specialist in Pune, I want all women to understand the symptoms and risk factors — so we can diagnose early and start treatment right away.
What Are the Symptoms of Endometrial Cancer?
The most common symptom of endometrial cancer is abnormal vaginal bleeding.
Watch for:
- Bleeding after menopause: Any vaginal bleeding that occurs a year or more after your last period is abnormal and should be evaluated immediately.
- Spotting between periods: Light bleeding or brownish discharge between menstrual cycles can be an early sign of endometrial changes.
- Heavy or prolonged periods: Menstrual bleeding that is unusually heavy, lasts longer than usual, or occurs more frequently than every 21 days may indicate a problem.
- Pelvic pain or pressure: Persistent lower abdominal pain or a feeling of fullness in the pelvis can suggest uterine abnormalities, including cancer.
- Pain during intercourse: Discomfort or pain during sex may result from changes in the uterine lining or inflammation, and should not be ignored.
- Unusual vaginal discharge: Watery, pink, or foul-smelling discharge — especially after menopause — can be a warning sign of endometrial cancer.
If you’re postmenopausal and notice any bleeding — even a little — please don’t ignore it. It may not always be cancer, but it must be evaluated.
What Increases the Risk?
Endometrial cancer often arises due to hormonal imbalances, particularly with excess estrogen. Knowing the risk factors allows women to take preventative or proactive measures.
Key Risk Factors Include:
- Age: Women over 50 are at a higher risk of developing endometrial cancer, as the likelihood increases with age, particularly after menopause.
- Obesity or Being Overweight: Excess body fat raises estrogen levels in the body, which can disrupt the hormonal balance and increase the risk of cancer in the lining of the uterus. Maintaining a healthy weight can significantly reduce this risk.
- Diabetes or High Blood Pressure: Chronic conditions like diabetes or high blood pressure are associated with an increased risk of endometrial cancer, possibly due to their connection with metabolic imbalances.
- Early Menstruation or Late Menopause: Starting menstruation before age 12 or entering menopause later increases the total years of exposure to estrogen, heightening the risk of developing cancer in the uterine lining.
- Never Being Pregnant: Women who have never experienced pregnancy are more exposed to consistent estrogen levels throughout their lives, unlike during pregnancy when estrogen levels fluctuate.
- Estrogen-Only Hormone Therapy: Using estrogen-only hormone replacement therapy (HRT), particularly after menopause, can increase the risk if not balanced with progesterone.
- Family History: A family history of endometrial or colon cancer may indicate a genetic predisposition, putting you at a higher risk of developing the disease.
- Genetic Factors: Inherited conditions like Lynch syndrome significantly increase the likelihood of endometrial cancer, along with other types of cancer, due to inherited gene mutations. Genetic counseling and testing may be helpful for women with a family history.
As an experienced Onco Surgeon in Pune, I also help women understand their genetic risk and offer screenings when needed.
How Is It Diagnosed?
Early diagnosis makes a huge difference in outcomes. If symptoms suggest endometrial cancer, we may recommend:
- Pelvic Examination: This is an initial physical exam where a healthcare provider checks for any visible or palpable abnormalities in the pelvic area, such as unusual swelling or tenderness, which may indicate potential concerns.
- Transvaginal Ultrasound: This imaging test involves inserting a small ultrasound probe into the vagina to get a detailed view of the uterus and surrounding structures. It is particularly useful for assessing the thickness of the endometrium (uterine lining). A thickened or irregular endometrium might suggest conditions such as polyps, fibroids, or even more serious issues that require further investigation.
- Endometrial Biopsy: During this procedure, a small sample of tissue is taken from the uterine lining. This tissue is then sent to a lab for analysis to detect any abnormalities, such as hyperplasia (overgrowth of cells) or cancerous changes. It is a key diagnostic step when abnormal uterine bleeding or other symptoms are present.
- Hysteroscopy: In this procedure, a thin, flexible camera (hysteroscope) is inserted through the cervix into the uterus, allowing the doctor to visually inspect the inside of the uterine cavity. This approach can help identify polyps, fibroids, or other structural issues that might not be detected through other methods.
- Dilation and Curettage (D&C): When a biopsy alone doesn’t provide enough clear information, a D&C may be performed. This involves dilating the cervix and gently scraping or suctioning tissue from the lining of the uterus. It provides a larger sample for analysis and can also help remove abnormal tissue.
- Imaging Scans (MRI/CT): If there are concerns about more complex conditions, such as the possibility of cancer spreading to other areas, advanced imaging scans like MRI or CT may be recommended. These scans provide detailed images of the uterus and surrounding tissues, aiding in diagnosis and treatment planning.
What Are the Stages of Endometrial Cancer?
Understanding how far the cancer has advanced informs the best treatment approach. Endometrial cancer is classified into four stages:
Stage I:
At this stage, the cancer is contained entirely within the uterus, meaning it has not yet spread to surrounding tissues or organs. It is often diagnosed early due to noticeable symptoms like abnormal bleeding or pelvic pain, which prompt medical attention.
This stage generally holds an excellent prognosis, and treatment usually involves surgery, such as a hysterectomy, and sometimes additional measures like hormone therapy to reduce the risk of recurrence.
Stage II:
In Stage II, the cancer has spread beyond the uterus and into the cervix, but it remains confined to the reproductive system. This stage is still considered localized, and treatment options typically include surgery, such as a hysterectomy, often combined with radiation therapy to ensure all cancerous cells are targeted.
In some cases, chemotherapy may also be recommended. With timely intervention, patients can achieve highly favorable outcomes.
Stage III:
By Stage III, the cancer has extended to nearby pelvic structures, such as the ovaries, fallopian tubes, or lymph nodes, but it has not yet reached distant organs. This stage often requires a more aggressive approach, typically involving a combination of surgery to remove as much of the tumor as possible, radiation to target any remaining cancer cells in the pelvic area, and chemotherapy to address potential microscopic spread.
Although the prognosis is more serious than earlier stages, advancements in treatment options continue to improve outcomes for many patients.
Stage IV:
Stage IV represents advanced cancer that has metastasized, or spread, to distant organs outside the reproductive system, such as the bladder, bowel, lungs, or liver. Treatment at this stage is more complex and often requires a personalized approach involving systemic therapies like chemotherapy, targeted drugs, or immunotherapy.
While a cure may not always be possible, these advanced therapies aim to control the disease, alleviate symptoms, and improve quality of life. In some cases, patients may still achieve positive outcomes, particularly with innovative treatments and clinical trials.
How Do We Treat Endometrial Cancer?
1. Surgery:
Surgery is the main treatment in most cases. It usually involves:
- Hysterectomy – removal of the uterus
- Bilateral salpingo-oophorectomy – removal of ovaries and fallopian tubes
- Lymph node dissection – to check if cancer has spread
As a surgical oncologist in Pune, I perform both traditional and minimally invasive surgeries, including robotic-assisted procedures when suitable. These often mean faster recovery and less pain.
2. Radiation Therapy:
Radiation may be recommended after surgery to reduce the risk of recurrence or if surgery isn’t an option.
It can be:
- External beam radiation therapy (EBRT)
- Internal radiation (brachytherapy)
Both are carefully planned to target cancer cells while minimizing damage to healthy tissue.
3. Hormonal Therapy:
Some endometrial cancers are hormone-sensitive. In these cases, progesterone-based pills or IUDs can help slow or stop the cancer’s growth, especially for women who wish to preserve fertility.
4. Chemotherapy:
Chemotherapy may be used for advanced stages or if cancer comes back. It works by killing fast-growing cancer cells throughout the body.
Though chemo can feel scary, we now have ways to manage side effects and support you through it.
5. Targeted Therapy & Immunotherapy:
These newer treatments are showing promise, especially in advanced or recurrent cases. Some target specific cancer mutations, while others help the immune system attack cancer.
Preventing Endometrial Cancer:
Although not all cases are preventable, simple lifestyle modifications can lower your risk:
- Maintain a healthy weight by focusing on a balanced diet and regular exercise, as obesity can increase the risk of endometrial cancer.
- Manage diabetes and high blood pressure effectively through medication, lifestyle changes, and routine checkups to reduce overall health risks.
- Discuss the potential risks and benefits with your doctor before starting hormone replacement therapy, as it may influence your risk of certain cancers.
- Treat abnormal bleeding promptly by consulting a healthcare provider, as it can be an early sign of endometrial issues that require attention.
- Consider using birth control pills after discussing with your doctor, as long-term use has been shown to lower the risk of endometrial cancer in some individuals.
- Stay consistent with pelvic checkups and screenings, particularly if you have a family history of gynecological cancers, to catch any issues early and maintain peace of mind.
Frequently Asked Questions (FAQ's):
Conclusion:
Endometrial cancer treatment isn’t just about surgery or medicine — it’s about trust, expertise, and compassionate care. With my experience as a dedicated Onco Surgeon in Pune, and the backing of Best cancer care clinic in pune, you’ll receive personalized, evidence-based treatment designed around you. Whether it’s a second opinion, early diagnosis, or a full treatment plan, you’re never alone in this journey.
Take the first step today. Let’s work together to protect your health and restore your peace of mind — with clarity, care, and confidence.
WhatsApp us
